Hospitals don't just manage costs — they manage outcomes, compliance, and trust. Financial misalignment in healthcare doesn't only affect margins. It affects patient care, regulatory standing, and operational continuity.
Healthcare finance operates under a different kind of pressure than most other industries. A delayed vendor payment in retail is an operational inconvenience. In a hospital, it can mean a supplier stops delivering critical consumables. A payout error in logistics affects a reconciliation report. In a hospital, it affects a doctor's trust in the institution they work within.
And yet, many hospital groups are still running financial operations built around manual approval hierarchies, post-spend reconciliation, spreadsheet-based payout tracking, and email-driven documentation. These systems were not designed for the scale, speed, or compliance requirements that modern multi-branch hospital networks face.
The gap is not between clinical teams and finance teams. It is between the speed at which hospitals need to operate and the infrastructure through which financial decisions currently flow.

The structural complexity that most systems underestimate
Multi-branch hospital networks manage financial flows that are genuinely more complex than most comparable organisations. At any given moment, the finance function is handling department-level advances, variable doctor incentives, procedure-based compensation, emergency vendor payments, pharmacy inventory purchases, biomedical equipment maintenance, and compliance obligations across multiple locations simultaneously.
Each of these categories moves at a different pace, involves different stakeholders, and carries different compliance implications. A system designed to handle a single financial category cleanly often breaks when asked to manage all of them together. The result is a finance team that spends most of its time in reactive mode — reviewing documents after money has moved, validating compliance after the fact, and correcting errors that a better-designed system would have prevented.
Doctor payouts: where precision matters most
Among all the financial flows in a hospital, doctor compensation is the most sensitive. It is also the most structurally complex. Modern doctor compensation models routinely combine revenue-sharing arrangements, incentive slabs tied to procedure volumes, case-based payouts, performance-linked bonuses, and ad-hoc reimbursements — often varying by department, seniority, and contract type.
When these calculations are managed manually, the risks compound quickly. Delays in payouts erode trust. Inconsistent calculations create disputes. Documentation gaps create audit vulnerability. And in a sector where the relationship between an institution and its clinical staff directly influences the quality of care delivered, none of these are purely financial problems.
Healthcare institutions do not just need faster payout processing. They need structured payout logic that is precise, transparent, and auditable at every step.
Embedding control before money moves
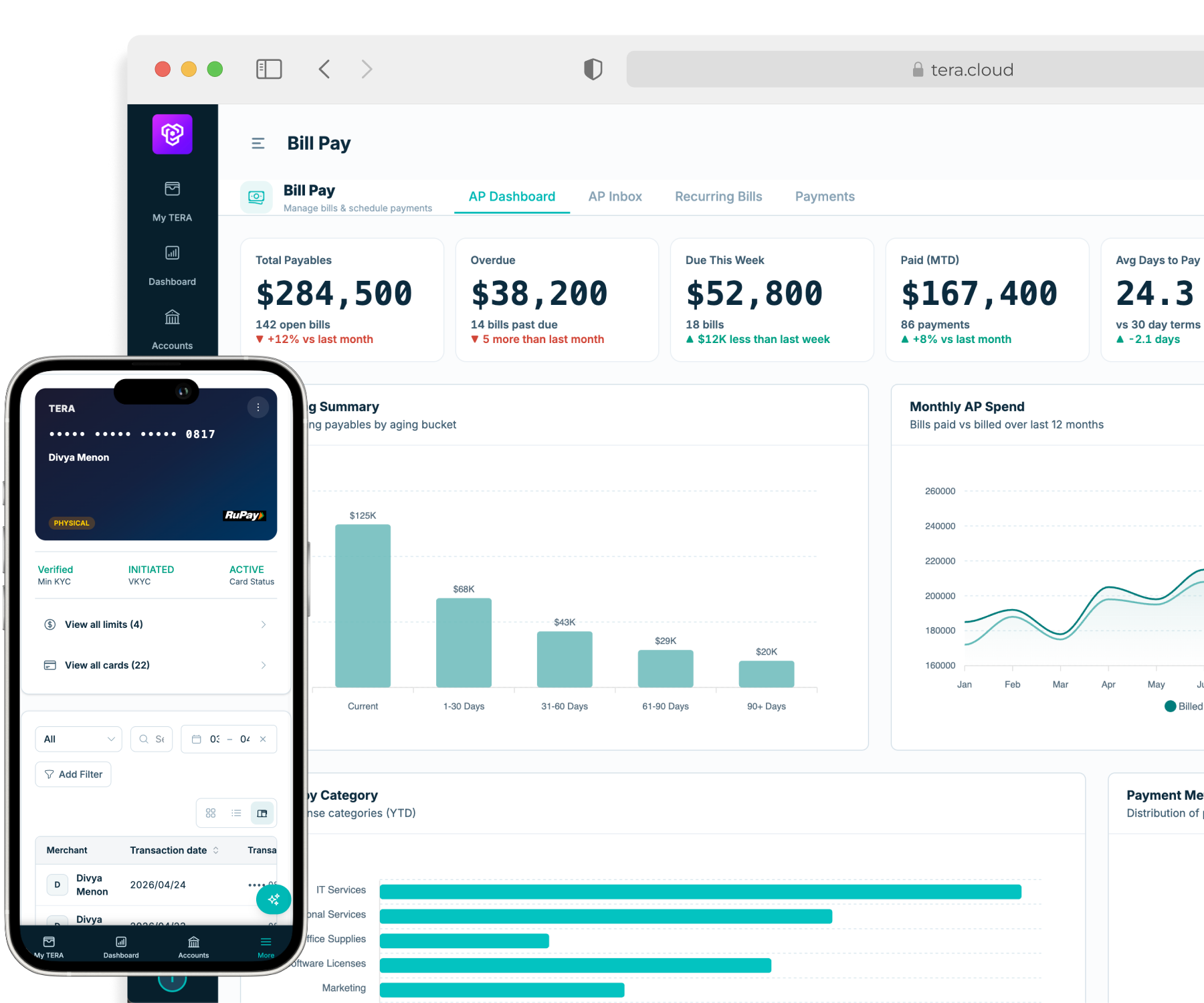
Forward-thinking hospital groups are rethinking this model. Rather than relying on post-spend checks and retrospective reconciliation, they are embedding financial controls directly into the transaction layer — so that policy is enforced at the point of payment, not discovered in the reporting cycle that follows it.
In practice, this means department budgets are pre-mapped and digitally enforced. Spend categories are predefined and restricted by cost centre. Doctor payouts follow structured calculation logic rather than manual worksheets. And before any payout or expense is processed, the system evaluates budget availability, cost centre alignment, policy compliance, and transaction consistency automatically.
Only when all conditions are satisfied are funds released. This removes dependency on retrospective checks and the manual corrections that follow them.
What changes for finance teams
The operational shift goes beyond efficiency. When pre-transaction validation replaces post-spend reconciliation, the finance team's role changes fundamentally. Instead of spending the majority of their time documenting what happened and correcting what went wrong, they move toward governing the system that makes things go right in the first place.
Payout accuracy improves. Reconciliation cycles shorten. Policy deviations decline. Department-level accountability becomes measurable rather than assumed. And finance teams recover the strategic bandwidth that manual processes have historically consumed.
Audit and compliance readiness as a by-product, not a project
Healthcare organisations operate under scrutiny from multiple directions simultaneously — regulatory bodies, insurance providers, accreditation authorities, and investors. In this environment, audit preparation is typically treated as a periodic, resource-intensive exercise. It should not be.
When financial controls are embedded into every transaction, audit readiness becomes a continuous state rather than a project that gets activated before an inspection. Every payment carries a clear audit trail. Documentation is generated automatically at the point of spend. Policy alignment is validated before funds are released, not verified after the fact.
The institutions that will handle increasing regulatory complexity most effectively are not those with the largest compliance teams. They are those whose financial infrastructure generates compliance evidence as a natural by-product of normal operations.
Closing perspective
Healthcare finance is not a back-office function. It is the infrastructure through which clinical operations are sustained. When it is reactive, slow, or opaque, those characteristics show up in the organisation's ability to pay suppliers on time, compensate doctors accurately, manage emergency procurement, and present a clean set of accounts to the people responsible for overseeing the institution.
The shift toward pre-transaction control and structured payout systems is not about replacing human judgment. It is about building a financial infrastructure that supports clinical speed, enforces institutional policy, and generates the kind of transparent, auditable record that modern healthcare governance requires.
If your hospital network operates across multiple locations and still depends heavily on manual approvals and post-spend reconciliation, the question worth asking is not whether you need a better system. It is how much the current one is costing you — in time, in errors, and in the trust of the people who depend on it working correctly.

.jpg)